
PACU Airway Assessment for LVNs
Postoperative patients require close monitoring of their airway and breathing. For a patient that has been given anesthesia the potiental complications can be easily avoided or promptly treated with good assessment skills. Patients come into the PACU in various stages of consciousness. Some patients are still intubated with the ETT and require mechanical ventilation. Some patients have the laryngeal mask airway (LMA) in place and are breathing on their own. Oral airways and nasal trumpets are common in the PACU to maintain airway integrity.
As a patient arrives in PACU, we immediately place the patient on an O2 supplement then put on the O2 sat monitor. As the monitors are placed, we are immediately assessing the patient’s respirations and skin color. The patient must have good air exchange in and out of the lungs. As in CPR, look for the chest to rise, listen for breath sounds, and feel for air coming out of the nose and mouth.
The Pulmonary System, PACU, & the Nurse
Factors affecting the pulmonary system of a postanesthesia patient are numerous. The ease of intubation and extubation are important in order to minimize the trauma to the airway. High humidity oxygen will be used if the intubation was difficult.
The type of surgery is a variable that affects the recovery in many different ways. For example, a thyroidectomy patient has the incision right at the neck which is a critical area if the patient were to bleed. A patient with a laparoscopy has experienced insufflation and subsequent diaphragmatic irritation which affects their breathing.
When a patient receives general anesthesia and has been given a neuromuscular blocking agent, it is important to assess muscle strength and the patient’s ability to take deep breaths, cough and clear their secretions. It is important to know if the patient was reversed or not. If the patient is very weak, then they might need more reversal of their neuromuscular blocking agent.
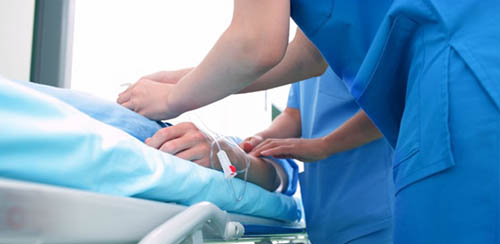
Assessment after Administering Meds in the PACU
The amount of narcotic administered to a patient is a key consideration to assess especially with relation to depth of respiration. If the patient hurts too much, they will not take deep breaths, and conversely, if they have too much pain medication then they will also not take deep breaths. Pain relief postoperatively is a delicate art. The patient needs to be comfortable, awake and breathing deeply all at the same time. Multiple modes of pain relief should include local, NSAIDS (if possible), and narcotics.
If the patient has received narcan it the immediate postoperative period, that patient needs to be observed in PACU longer in order to ensure that the patient will not resedate. Narcan should be titrated in 40mcg increments until the desired effect is reached. The patient needs to be observed because narcan is shorter acting than the narcotic that is is reversing.
One very dangerous airway complication is laryngospasm. It is characterized by spasm of the vocal cords which blocks the flow of air into the lungs. Patients with laryngospasm move restricted amounts of air or sometimes no air movement at all. Laryngospasm is treated by bagging the patient with positive pressure. If this is not successful then succcinylcholine should be given to paralyze the patient and break the spasm. When the succinylcholine wears off, the patient should be placed on high humidity oxygen and be assessed for several hours for pulmonary edema.

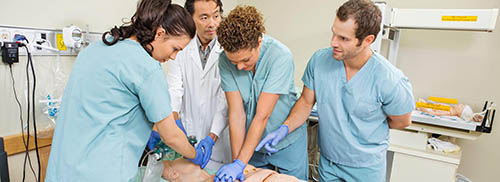
Why LVNs Need to do Airway Assessments
Therapeutic nebulizer treatments are used to help patients breath easier. The patient presenting with stridor (upper airway constriction) will receive racemic epinephrine in a neb to reduce edema and open that airway. Patients with stridor are at risk for laryngospasm. Those patients coughing and wheezing need a bronchodilator like albuterol to help them.
Deep breathing is an important process in the recovery from anesthesia. Patients that are having a difficult time doing this on their own will benefit from an incentive spirometer. The incentive spirometer gives the patient a goal and a structured way to complete the deep breathing.
Airway assessment is the primary concern when a patient is delivered from the operating room. By using assessment skills and critical thinking processes, each patient will have the very best outcome.
How Much do PACU LVNs Make?
The salary of a PACU nurse depends on many things: years of experience, location, and which shift is worked. By browsing through sites such as Indeed.com, we can see the average LVN salary for a nurse with 2 years of post surgical experience is approximately $54,000 per year. There are, however, some issues to keep in mind. In some states, LVNs aren’t allowed to do IV pushes, which would severely inhibit their ability to work in a PACU.
Before applying for a postoperative nursing position, be sure to check out your state’s nurse licensing body to verify your scope of practice. You don’t want to go through all the trouble of applying for a position, interviewing, putting in your salary expectations, only to find out vocational nurses can’t titrate drips, push IV meds, etc!

 Follow
Follow